
- Home
- Who We Are
- Treatment Programs
- What We Treat
- Resources
- Get Started
If you find yourself searching for “anxiety treatment near Cincinnati” (or “anxiety treatment near me”), it’s likely not a casual endeavor.
Typically, it signifies a moment of urgency:
This guide aims to simplify your search and make it less overwhelming.
We’ll explore the primary anxiety therapy options available in Cincinnati and Southwest Ohio, clarify what different levels of care entail (outpatient, intensive programs, inpatient), provide insight into what an assessment typically involves, guide you on how to choose a suitable program, and outline what to expect from the initial day of treatment through to aftercare.
It’s crucial to understand that anxiety treatment is not one-size-fits-all. The ideal approach varies based on symptom severity, safety risk, the extent to which anxiety impacts daily functioning, and whether there are co-occurring issues such as depression, trauma, or substance use.
While stress is a normal part of life, anxiety disorders represent a different realm altogether.
To differentiate between the two: stress is usually linked to a specific situation and tends to diminish once that situation passes. In contrast, an anxiety disorder tends to linger, manifesting across various aspects of life and influencing decisions through avoidance, constant worry, or seeking reassurance.
Anxiety becomes clinically significant when it transcends occasional nerves and begins to involve:
Some common anxiety disorders include:
If you’re seeking reliable education alongside treatment for your anxiety disorder, consider exploring these reputable resources:
However, if your anxiety is significantly impacting your sleep patterns, relationships, academic performance or work productivity, it’s a clear indication that you should seek professional support rather than merely attempting to “push through”. For those located in the Cincinnati area seeking immediate assistance with their anxiety symptoms or looking for mental health treatment near Cincinnati, Cedaroaks Wellness can provide the necessary support.
Anxiety can be loud and obvious, like a panic attack. It can also be quiet and constant, like nonstop worry in the background. Many people experience a mix.
Emotional and cognitive symptoms may include:
Physical symptoms may include:
Behavioral signs may include:
If any of the below are happening, it’s important to get evaluated right away:
If you’re in immediate danger, call 988 (Suicide & Crisis Lifeline) or go to the nearest ER.
Anxiety disorders are among the most common mental health conditions. Organizations like NIMH and ADAA consistently report high lifetime and yearly prevalence, and most clinicians will tell you the same thing from experience: anxiety is everywhere, and it’s incredibly disruptive when it goes untreated.
The tricky part is that anxiety often convinces people to wait.
It whispers things like:
But “waiting it out” can come with real costs:
The hopeful truth: anxiety is treatable, and earlier support often means quicker stabilization and fewer life disruptions.
You don’t need a “perfect” reason to get help. You just need enough awareness to say: this isn’t working anymore.
Professional anxiety treatment is worth considering when:
This is also where the idea of the right level of care matters. Some people can start with outpatient therapy and do great. Others need more support because functioning or safety is compromised.
And if substance use is part of the picture, that matters too. Co-occurring conditions often require integrated planning, not separate treatment tracks that don’t talk to each other.
When people say “anxiety treatment,” they might mean a few different things. Here’s a practical breakdown.
This usually looks like:
Outpatient can be a great fit if you’re generally safe and functioning, even if you feel miserable inside.
These are often designed for moderate-to-severe symptoms or situations where weekly therapy isn’t enough. Programs vary, but commonly include:
This level can help when anxiety is disrupting daily life, but you’re still able to live at home safely. Dialectical Behavior Therapy (DBT) is one such intensive option that has shown effectiveness in treating anxiety and related disorders.
Inpatient care is the highest level of support. It’s typically recommended when:
Most decisions come down to:
In the Cincinnati area, many people also look across Southwest Ohio for availability and clinical fit, especially when symptoms feel urgent and waitlists are long.
Anxiety treatment works best when it’s practical, skills-based, and tailored to your specific anxiety pattern.
Here are common components you might see in a treatment setting:
This is where you:
A big part of anxiety recovery is learning to respond differently, not just feel better in the moment. Techniques like Cognitive Behavioral Therapy (CBT) are often utilized for this purpose.
Group therapy can be surprisingly powerful for anxiety because it:
Family support can help anxiety recovery a lot, especially when loved ones (with the best intentions) accidentally reinforce avoidance or reassurance loops. Family sessions can focus on:
Not every anxiety tool is a worksheet. Structured activities can help:
Most treatment plans include a combination of these therapies, adjusted to the diagnosis and the level of care.
If you’ve never had a real intake evaluation, it can feel intimidating. Most people worry they’ll be judged, dismissed, or told they’re “overreacting.”
A good intake is the opposite. It’s about clarity and a plan.
A typical evaluation includes:
Clinicians may also work to clarify whether symptoms best match:
Ideally, the outcome is:
A strong anxiety plan is specific, measurable, and realistic.
Most plans include:
Depending on your symptoms, you may work on:
Many programs track progress with simple tools:
As you stabilize, the level of care can step down. If symptoms spike or safety changes, the plan may step up. The goal is to match support to what you actually need, not keep you in a rigid box.
Anxiety and substance use often reinforce each other.
A common pattern looks like:
This is why treating only one side can backfire:
Integrated care typically includes:
At Cedar Oaks Wellness Center, we specialize in substance use disorders and co-occurring mental health conditions, including anxiety. We offer detox and inpatient programs in a supportive, structured environment, with personalized planning from intake through aftercare.
Not knowing what treatment will be like is a huge barrier. Anxiety hates uncertainty, so let’s make this part clearer.
While schedules vary by program, many days include:
You’re not doing this alone. Treatment usually includes:
It’s completely fair to ask about practical details like:
This is normal and important to expect. Most people have ups and downs. Anxiety recovery is a lot of repetition, practice, and gradually doing what anxiety tells you to avoid, in a safe and supported way.
Aftercare is where progress becomes sustainable.
An aftercare plan may include:
Recovery goes better when the people around you understand the plan. Aftercare often involves:
Incorporating family therapy into your aftercare can enhance understanding and support from your loved ones.
This usually includes:
In Ohio, practical factors like scheduling, transportation, and access can make or break follow-through. Aftercare helps solve those issues before you’re back in the real world trying to figure it out on a bad day.
When you’re comparing options, it helps to have a simple checklist.
If you’re comparing facilities, some people also look at hospital-based options in the region. The best choice depends on clinical fit, symptom severity, and the intensity of support you need, not just what’s closest.
If you’re unsure whether outpatient or inpatient makes more sense, a short screening call can often clarify the next right step.
Located in Oregonia, Ohio, Cedar Oaks Wellness Center is easily accessible for those seeking anxiety treatment near Cincinnati and throughout Southwest Ohio.
We specialize in comprehensive treatment for substance use disorders and co-occurring mental health conditions, including anxiety. Our offerings include detox and inpatient programs within a supportive, structured environment.
Our approach is personal, not cookie-cutter. We tailor treatment to each client’s needs, experiences, and recovery goals, with coordinated planning that starts at intake and continues through discharge and aftercare.
You may be a strong fit for Cedar Oaks if:
You don’t have to have everything figured out to reach out. You can start with a conversation about what’s been going on, and we can help sort through your options and determine the right level of care.
If you’re in immediate danger or having suicidal thoughts, call 988 or go to the nearest ER.
For those seeking anxiety treatment near Cincinnati with support for co-occurring substance use or a higher level of structured care, we invite you to contact us at Cedar Oaks Wellness Center. You can easily schedule an assessment to discuss your situation and explore potential next steps.
Finding the right anxiety treatment near Cincinnati can be challenging due to escalating symptoms, urgency for professional help, uncertainty about therapy or medication needs, and generic information on many websites. This guide simplifies the process by clarifying therapy options, levels of care, assessments, program selection, and treatment expectations.
Stress is typically linked to specific situations and diminishes once those situations pass. Anxiety disorders persist over time, affect multiple life areas, involve avoidance behaviors or constant worry, and cause distress that feels unmanageable despite rational understanding.
Symptoms include excessive worry, irritability, racing thoughts, chest tightness, shortness of breath, muscle tension, sleep disruption, avoidance of places or people, reassurance seeking, compulsive checking, and using substances to cope. Persistent symptoms impacting daily functioning suggest an anxiety disorder.
Seek immediate evaluation if you experience suicidal thoughts, inability to function (not eating or sleeping), severe panic attacks that feel unmanageable, psychosis symptoms like hearing voices or paranoia, self-harm risk, or unsafe substance withdrawal. In emergencies, call 988 or visit the nearest ER.
Anxiety disorders are highly prevalent and disruptive when untreated. Early treatment prevents worsening symptoms and impairment in work, school, relationships, and overall quality of life. Delaying care often occurs due to minimizing symptoms or waiting for a less busy time, but can lead to increased distress.
Reliable resources include Cedaroaks Wellness website offering mental health support in the Cincinnati area; National Institute of Mental Health (NIMH); Anxiety and Depression Association of America (ADAA); and National Alliance on Mental Illness (NAMI). Cedaroaks Wellness also provides assessment and tailored treatment programs.
Trying to figure out mental health treatment in Ohio can feel like opening 20 browser tabs and still not knowing what to do first. Between different program types, insurance rules, and the very real stress of not feeling okay, it’s easy to get stuck.
This guide is here to make it simpler. We’ll walk through the main levels of care in Ohio, what different programs treat, what therapy and psychiatry often look like, and how to choose the right fit. And if you’re also dealing with substance use, we’ll cover how integrated, co-occurring care works because mental health and addiction are often connected.
A lot of people hit the same barriers, even when they’re motivated to get help:
So what does good care actually look like, no matter where you go?
High-quality mental health treatment usually includes:
It’s also important to know this: mental health and substance use often overlap. Anxiety can fuel drinking. Depression can worsen after stimulant or opioid use. Trauma symptoms can drive relapse. When both are present, treating them together (not in separate silos) usually improves outcomes.
If symptoms are severe, you may need a higher level of care sooner than you expected. Examples include:
In those moments, it’s not “too much” to seek intensive help. It’s the right move.
Think of treatment like a ladder. People move up or down based on symptoms, safety, medical needs, and how much support they have at home.
Here’s the most common continuum of care you’ll see in Ohio:
Who it’s for: People who are safe at home and able to function day-to-day, but need support for mental health symptoms, stress, trauma, relationships, or substance use recovery.
What it looks like:
What it can treat: Anxiety, depression, PTSD, grief, mild-to-moderate substance use issues, relationship issues, and more. Outpatient is also common as step-down care after inpatient/residential.
Ohio programs often offer IOP and PHP as a middle level between standard outpatient and inpatient/residential.
These are good options when weekly therapy is not enough but 24/7 care is not required. For those who find themselves in such situations, resources like Cedar Oaks Wellness can provide the necessary support and guidance through these mental health programs.
People mix these terms up all the time, so here’s a clean distinction.
Inpatient treatment generally means:
Residential treatment generally means:
In plain English, inpatient care often helps you get stable. Residential often helps you get better and build a foundation.
A residential treatment facility is a live-in program where your day is structured around recovery.
People often benefit from residential care when they:
Daily programming often includes:
Detox is necessary when someone is at risk for dangerous or severe withdrawal, most commonly from:
Detox helps with medical monitoring and stabilization, but detox alone is not full treatment. The real progress usually happens when detox is followed by inpatient/residential care or a structured outpatient plan.
Ohio programs treat a wide range of mental health conditions, and many people have more than one diagnosis at the same time.
It may be time to seek help if you notice:
Common care approaches include:
Accurate diagnosis matters here because treatment can look very different than depression treatment.
Care often includes:
Many people with personality disorder symptoms benefit from consistency, structure, and skills-based treatment.
Care often includes:
Substance use and mental health symptoms often reinforce each other. For example:
Integrated treatment focuses on both sides at once, not “get sober first, then we’ll talk about mental health later.”
If you’re comparing programs, it helps to know what these therapies actually look like in real life.
In individual sessions, you can expect:
CBT is based on the idea that thoughts, feelings, and behaviors are connected.
It often includes:
Groups help because you get:
A typical group schedule might include process groups, skills groups, psychoeducation, and recovery-focused groups.
Moreover, for individuals dealing with PTSD or trauma, these therapies can be particularly beneficial. They provide a safe space to address underlying issues while also equipping individuals with the necessary tools to manage their symptoms effectively.
Family sessions can help with:
Family involvement is not always appropriate, especially when relationships are unsafe or actively harmful. Good programs make room for that reality.
Medication can be helpful, but it should never feel like a rushed decision or a “one-and-done” appointment.
Quality medication management includes:
If addiction is part of the picture, choosing a program that understands co-occurring needs can make a huge difference.
Some facilities focus primarily on addiction. Others focus primarily on mental health. The best fit for many people with dual diagnosis is a program that can treat both in an integrated way.
Integrated programming is ideal when you’re dealing with:
Detox typically includes:
The key question to ask is: What happens after detox? A strong program plans the next step from day one.
MAT is the use of FDA-approved medications to support recovery, commonly for:
MAT works best alongside therapy, recovery planning, and mental health treatment when needed.
Good treatment doesn’t just focus on stopping use. It focuses on staying well.
Relapse prevention planning often includes:
Inpatient or residential care may be the safer option if you have:
Holistic supports can be genuinely helpful, as long as they’re framed correctly.
The simplest way to think about holistic care is this: add-on supports, not replacements for evidence-based treatment.
Supportive options you may see include:
Some centers also offer complementary services like acupuncture or massage therapy. These can support stress reduction, body awareness, and emotional regulation during early recovery.
Be cautious with programs that:
Holistic supports are at their best when they help you engage with CBT/DBT skills and stay regulated enough to do the deeper work.
Choosing a program can feel like a big decision because it is one. Here are practical things to look for.
Licensing and accreditation matter because they’re basic indicators of safety standards, staffing expectations, and accountability.
Ask:
Questions worth asking on the phone before you commit:
You want a program that plans for life after discharge.
Look for:
These details matter more than people expect:
Be cautious if you hear:
There isn’t one “correct” length of stay. It can vary based on:
The goal is not to keep you in treatment longer than necessary. The goal is to get you stable, build skills, and set you up with a plan you can realistically follow.
Early days typically focus on:
While schedules vary, many programs include:
Real progress often looks like:
Stepping down is part of the process, not an afterthought. Many people transition from:
Follow-up appointments matter a lot here. The gap after discharge is when people can feel most vulnerable, so continuity is key.
Cost can vary widely depending on:
Here are a few terms you’ll hear often:
When you call to check coverage, it helps to have:
Ohio has state and community resources through the Ohio Department of Behavioral Health. State resources can be helpful for:
If you’re waiting for care, you can still take steps now:
At Cedar Oaks Wellness Center, we’re a comprehensive treatment provider in Oregonia, Ohio, specializing in substance use disorders and co-occurring mental health conditions. We offer detox and inpatient programs in a supportive, structured environment designed for stabilization and real momentum in recovery.
Here’s what that means in practice:
You may be a good fit for our care if you’re looking for:
If you’re concerned about how to manage your insurance coverage during this process, it’s worth noting that we provide guidance on navigating insurance verification, ensuring that you have the necessary support when seeking treatment.
If you’re not sure what to do next, here’s a simple action plan:
And please don’t wait for “rock bottom.” If depression or anxiety is worsening, substance use is escalating, or safety concerns are showing up more often, that is reason enough to reach out.
If you’re considering detox, inpatient support, or dual diagnosis treatment in Ohio, contact us at Cedar Oaks Wellness Center today. Call us at 513-654-9978. We’ll talk through what’s going on, help you understand your options, verify insurance, and schedule an assessment so you can take the next step toward stability and recovery.
Ohio offers a continuum of mental health care levels, including outpatient therapy, Intensive Outpatient Programs (IOP), Partial Hospitalization Programs (PHP), inpatient treatment, and residential treatment. These levels range from weekly therapy sessions to 24/7 live-in care depending on the individual’s symptoms, safety needs, and support system.
Outpatient therapy is suitable for those who are safe at home and able to function day-to-day but need support for symptoms like anxiety, depression, or mild-to-moderate substance use issues. If weekly sessions aren’t enough, programs like IOP or PHP offer several days per week of more intensive care without requiring 24/7 supervision. Severe symptoms or safety concerns might require inpatient or residential treatment.
Inpatient treatment in Ohio involves 24/7 medical supervision, typically in a hospital setting, focused on stabilization, safety, detox support, and managing acute symptoms. Residential treatment also provides 24/7 live-in care but emphasizes structured daily programming such as therapy, skill-building, routine establishment, relapse prevention, and longer-term recovery work.
Integrated co-occurring care treats mental health conditions and substance use disorders simultaneously rather than separately. This approach improves outcomes because conditions like anxiety can fuel substance use, and trauma can drive relapse. Programs often combine evidence-based therapies such as CBT or DBT with medication management and relapse prevention tailored to both diagnoses.
Good mental health care includes a thorough assessment beyond a quick intake; an individualized treatment plan based on your specific symptoms and goals; evidence-based therapies like CBT or trauma-informed approaches; appropriate medication support with monitoring; coordinated care when multiple diagnoses exist; and clear, measurable goals to track progress.
Navigating mental health treatment in Ohio can feel confusing due to multiple program types, insurance complexities like prior authorizations and coverage limits, stigma around seeking help, long waitlists, especially for psychiatry, and many unfamiliar acronyms (IOP, PHP). To overcome this, start with a trusted provider who offers guidance through available options tailored to your needs and ensures coordination of care.
At Cedar Oaks Wellness Center, we have always operated under the guiding principle that mental health is not just “in your head”, it is a profound physiological experience that can be significantly enhanced through IV therapy. The brain, while responsible for our thoughts and emotions, is an organ that requires a specific, high-quality fuel set to function at its peak. When we navigate the heavy lifting of recovery, manage chronic stress, or deal with mental health challenges, our bodies often deplete vital nutrients much faster than we can replenish them through diet alone.
Starting today, March 5, 2026, we are thrilled to expand our holistic toolkit with the official launch of the Brain Boost IV. Specifically formulated with our Mental Health Day Treatment clients in mind, this advanced IV therapy is designed to bridge the functional gap between physical biology and emotional stability.
We believe so strongly in the impact of integrated, holistic care that we want as many of our clients as possible to feel the difference for themselves. To celebrate the launch of this new service, we are offering an Introductory Special of $99 per treatment.
This is an invitation to invest in your cognitive health and give your mind the “reset” it deserves. Recovery is about more than just surviving; it is about thriving.

Our clinical team meticulously selected a specific blend of ingredients known for their profound impact on the “brain-body connection.” The Brain Boost IV isn’t just about general health; it’s about targeting the specific pathways that regulate mood, focus, and stress.
B vitamins are the essential building blocks of a healthy brain. They play a critical role in cellular energy production and the synthesis of neurotransmitters—the chemicals that allow brain cells to communicate. By providing a full spectrum of B vitamins, we help nourish the brain’s ability to maintain focus and promote a steadier, more resilient sense of well-being throughout the day.
In the world of wellness, magnesium is frequently referred to as “nature’s relaxant.” It is vital for nervous-system balance and plays a key role in deactivating the “fight or flight” response. For clients experiencing high anxiety or physical restlessness, magnesium helps support muscle release and deep relaxation, encouraging a more centered emotional state that makes therapeutic work more accessible.
B12 is a powerhouse nutrient for cognitive function and natural energy production. It is essential for the health of nerve tissue and brain function. By supporting emotional balance and stabilizing mood, B12 helps clear the “mental static” that often contributes to feelings of depression or overwhelm, ensuring the brain has the energy it needs to process complex emotions.
The Brain Boost IV is more than just a nutrient replenishment; it is a clinical intervention designed to be a supportive partner to your daily mental health work. When your brain is physically starved of the nutrients it needs to regulate cortisol (the stress hormone), even the best therapy sessions can feel like an uphill battle. By stabilizing your internal chemistry, you are better equipped to engage in the work of healing.
Key benefits you may experience include:
While we are proud to offer this service to our broader community, the Brain Boost IV was specifically curated for our mental health day treatment clients. We understand that the work done in intensive mental health programming, the deep-diving into trauma, the skill-building, and the emotional processing, is physically and mentally taxing.
Providing your brain with physiological support allows you to show up more fully for your sessions. It gives you the “bandwidth” to listen, learn, and implement the tools our clinicians provide. We want you to have every possible advantage as you rebuild your life, and that starts with a healthy, well-nourished brain.
Many people rely on oral multivitamins to support their health, and while these are beneficial, they are often limited by the human digestive system. When you swallow a pill, it must be broken down by stomach acid and processed by the liver before it ever reaches your bloodstream. During this process, a significant percentage of the nutrients are lost—a concept known as low bioavailability. Furthermore, for those struggling with high stress or gut health issues, absorption rates can drop even lower.
IV therapy changes the equation. By bypassing the digestive tract entirely, the Brain Boost IV delivers a soothing blend of brain-supportive nutrients directly into your system for 100% bioavailability. This ensures that your nervous system receives the exact concentration of vitamins it needs to begin the repair process almost instantly. It provides a biological “reset,” allowing your mind to quiet down and your body to settle.
Visit the front desk at Cedar Oaks Wellness Center today or speak with your primary clinician to see if the Brain Boost IV is right for your treatment plan. Let’s fuel your recovery from the inside out and revitalize your spirit for the road ahead.
In the journey toward wellness and recovery, we often focus intensely on the mind—processing thoughts, addressing trauma, and relearning behaviors. However, true healing is a “whole-body” experience. At Cedar Oaks Wellness Center in Cincinnati, Ohio, we believe in integrating holistic modalities that ground the body and soothe the nervous system.
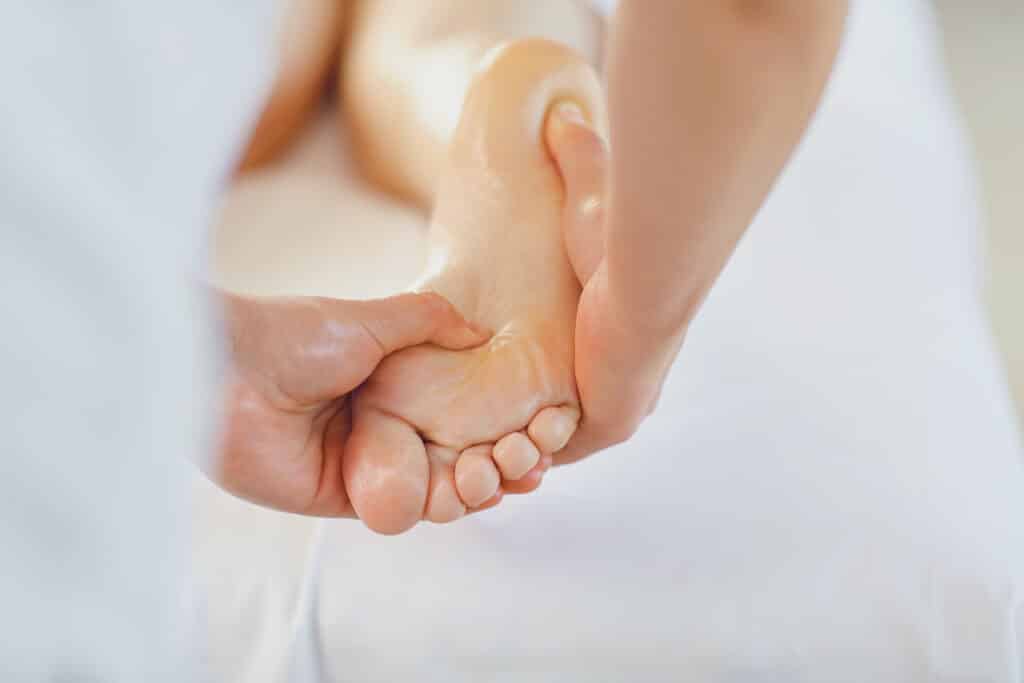
One of the most effective tools in this integrated approach is Reflexology Therapy. While it may look like a simple foot massage to the untrained eye, reflexology is a sophisticated clinical practice that maps the entire body through specific pressure points. In this guide, we explore how reflexology therapy in Ohio is helping our clients reconnect with themselves and find lasting peace.

Reflexology is a therapeutic method that involves applying gentle, focused pressure to specific points on the feet (and sometimes the hands) that correspond to various organs and systems within the body. By stimulating these “reflex zones,” a practitioner can encourage the body’s natural healing processes.
For individuals in recovery, reflexology acts as a bridge between physical comfort and emotional stability. Many clients at our Ohio campus report feeling a profound sense of “grounding” after a session, as the focused pressure helps draw their awareness away from racing thoughts and back into their physical form.
When navigating the early stages of addiction recovery or mental health treatment, the body is often in a state of high alert. Reflexology therapy in Ohio offers a non-invasive way to “reboot” the system.
At Cedar Oaks Wellness Center, we don’t view reflexology as a “luxury” or a spa treatment. Instead, it is an essential thread in our therapeutic tapestry. Our serene, wooded campus in the Greater Cincinnati area provides the perfect backdrop for this type of sensory healing.
We integrate reflexology with traditional evidence-based treatments, such as Cognitive Behavioral Therapy (CBT) and group counseling. This ensures that while you are doing the hard work of mental processing, your body is being supported and nurtured simultaneously.
If you find yourself feeling disconnected, physically tense, or emotionally overwhelmed, reflexology may be the “missing piece” in your wellness plan. While traditional therapy addresses the cognitive aspects of recovery, reflexology works from the “bottom up,” using the nervous system to communicate safety to the brain. This practice is particularly effective for individuals who are navigating the high-stress environment of early sobriety or managing long-term mental health challenges.
Reflexology therapy is often a successful intervention for those who:
Recovery is about more than just “stopping” a behavior; it’s about starting a new way of living. At Cedar Oaks Wellness, we are dedicated to providing the residents of Ohio and the surrounding regions with the highest standard of compassionate, comprehensive care.
If you are ready to explore how reflexology therapy and our other integrated programs can help you reclaim your life, reach out to our team today.
Dual diagnosis refers to the simultaneous presence of a substance use disorder and a mental health condition. When someone struggles with both addiction and a mental health challenge like depression, anxiety, or PTSD, they need specialized care that addresses both issues at the same time. This integrated approach is essential because these conditions often feed into each other, creating a cycle that’s difficult to break without proper support.
The complexity of treating co-occurring disorders cannot be understated. Substance use can mask or worsen mental health symptoms, while untreated mental health conditions may drive someone to self-medicate with drugs or alcohol. This intertwined relationship means that treating only one condition while ignoring the other rarely leads to lasting recovery.
Common co-occurring conditions include:
The challenges in treating both conditions together are significant:
Finding a dual diagnosis treatment center that understands these complexities and offers truly integrated care becomes not just important—it’s essential for healing and long-term wellness.
Such centers provide dual diagnosis treatment programs that cater to the unique needs of individuals facing these overlapping challenges, ensuring comprehensive care that promotes recovery from both substance use disorders and mental health conditions simultaneously.

When searching for a licensed dual diagnosis center, accreditation serves as your first line of protection. Think of it as a seal of approval from independent organizations that have thoroughly evaluated the facility’s practices, staff qualifications, and treatment protocols.
Accredited rehab facilities have undergone rigorous review processes by respected organizations such as:
Joint Commission accreditation and CARF certification mean that a treatment center has demonstrated its ability to provide integrated care for both substance use disorders and mental health conditions. These organizations don’t simply check boxes—they examine how facilities coordinate psychiatric care with addiction treatment, how they train their staff, and whether they follow evidence-based practices.
Licensing goes beyond accreditation by ensuring legal compliance with state regulations. A properly licensed facility has met minimum safety standards, maintains appropriate staff-to-client ratios, and operates under regular oversight. Without proper licensing, a facility may lack qualified medical professionals, adequate emergency protocols, or appropriate medication management—all critical components when treating complex dual diagnosis cases.
Healing from co-occurring disorders takes time—often more than many people initially expect. When you’re addressing both addiction and mental health conditions, your brain and body need adequate time to process, heal, and develop new patterns of thinking and behavior. The length of stay dual diagnosis programs offer can significantly impact your chances of lasting recovery.
Extended rehab programs of 90 days or longer provide several distinct advantages:
Short-term programs lasting 30-40 days can provide initial stabilization and introduce you to recovery concepts. However, they rarely allow sufficient time to address the underlying causes of both conditions or to practice new skills until they become automatic responses. For instance, substance abuse and mental health issues often intertwine, making it essential to delve deep into both areas during treatment.
For dual diagnosis treatment, think of the journey as a marathon rather than a sprint—giving yourself the gift of time can make the difference between temporary relief and genuine transformation. It’s crucial to understand that the length of stay in dual diagnosis programs plays a vital role in ensuring comprehensive recovery.
When searching for the right dual diagnosis treatment center, the availability of a continuum of care dual diagnosis approach becomes essential to your healing journey. This means the facility should offer multiple levels of treatment that can adapt as your needs change throughout recovery.
Detoxification services serve as the critical first step for many people beginning treatment. Withdrawal symptoms can range from uncomfortable to potentially dangerous, depending on the substances involved and the severity of use. A treatment center with medical detox capabilities provides:
Following detox, access to inpatient rehab programs becomes the foundation for deeper healing. Residential treatment offers a structured, supportive environment where you can focus entirely on recovery without the distractions or triggers of daily life. The best facilities tailor these programs to address your specific combination of mental health and substance use challenges, recognizing that your path to wellness is uniquely yours.
A true continuum also includes step-down levels of care—partial hospitalization and intensive outpatient programs—allowing you to gradually transition back into everyday life while maintaining strong therapeutic support.
The foundation of effective dual diagnosis treatment rests on evidence-based behavioral therapies that address the intricate connection between mental health and substance use. When exploring treatment centers, ask specific questions about their therapeutic approaches and the qualifications of those delivering care.
Cognitive Behavioral Therapy (CBT) helps you identify and reshape the thought patterns that fuel both addiction and mental health struggles. This approach teaches practical skills to manage cravings, recognize triggers, and develop healthier coping mechanisms. For someone dealing with depression and alcohol dependence, CBT provides tools to challenge negative thinking while building resistance to substance use.
Dialectical Behavior Therapy (DBT) offers particularly powerful benefits for those experiencing intense emotions, trauma responses, or conditions like borderline personality disorder alongside addiction. This therapy focuses on four key areas:
Individual counseling with licensed therapists creates space for deeply personalized work. These one-on-one sessions allow you to explore your unique story, uncover underlying trauma, and develop a recovery plan that honors your specific needs. The therapeutic relationship itself becomes a healing experience, offering consistent support as you navigate the complexities of dual diagnosis recovery.
Quality treatment centers employ therapists specifically trained in both addiction and mental health, ensuring you receive integrated care rather than fragmented approaches.
Integrated care dual diagnosis represents a fundamental shift from traditional treatment models that address addiction and mental health as separate issues. When these conditions receive simultaneous, coordinated attention, healing becomes more comprehensive and sustainable. Think of it like treating both sides of the same coin rather than flipping between them—your recovery team sees the complete picture of how your struggles interconnect.
The strength of this approach lies in the collaboration between diverse specialists working together under one roof:
This coordination means your psychiatrist knows what your therapist discussed in your morning session. Your addiction specialist understands which medications you’re taking. Everyone communicates regularly about your progress, challenges, and evolving needs. This unified approach prevents conflicting treatment recommendations and ensures every professional supporting you shares the same goals for your recovery journey.
At Cedar Oaks Wellness Center, this collaborative model creates a safety net where nothing falls through the cracks, and you receive truly holistic treatment that honors the complexity of your experience. Such an integrated multidisciplinary treatment approach is essential for addressing the intricate interplay between mental health and substance use disorders effectively.
When searching for how to choose a dual diagnosis treatment center: a 5-point checklist, understanding the specific advantages of specialized care becomes essential. The benefits dual diagnosis program at Cedar Oaks Wellness Center offers extend far beyond standard addiction treatment.
Comprehensive personalized care forms the foundation of effective dual diagnosis treatment. At Cedar Oaks, treatment plans are crafted around each person’s unique circumstances, recognizing that your journey with co-occurring disorders differs from anyone else’s. This individualized approach means your treatment team considers your specific mental health symptoms, substance use patterns, personal history, and recovery goals when designing your path forward.
The focus on addressing root causes sets dual diagnosis programs apart from traditional addiction treatment. Rather than simply managing symptoms or achieving temporary sobriety, Cedar Oaks’ approach digs deeper to understand what drives both conditions. Perhaps unresolved trauma fuels both anxiety and substance use, or maybe depression creates vulnerability to addiction. By identifying and treating these underlying factors, the program helps prevent the cycle of relapse that often occurs when only surface-level symptoms receive attention.
The 120-acre campus near Cincinnati provides a healing environment where you can focus entirely on recovery, supported by state-of-the-art facilities and evidence-based therapies like DBT and CBT that specifically target the complex relationship between mental health and addiction.
Completing a treatment program marks the beginning of a lifelong journey, not the end. The aftercare dual diagnosis recovery at Cedar Oaks Wellness Center provides the foundation you need to maintain the progress you’ve worked so hard to achieve. When you’re managing both a mental health condition and substance use disorder, the transition back to daily life can feel overwhelming without proper support systems in place.
Cedar Oaks recognizes this reality and offers lifetime aftercare for all alumni, ensuring you’re never alone in your recovery journey. Through the Cedar Oaks Cares alumni app, you maintain connection with your support network, access resources when challenges arise, and stay engaged with a community that understands your experience.
Continuing therapy sessions after leaving the facility helps you navigate new situations and stressors using the coping skills you’ve developed. Whether you’re facing relationship challenges, work pressures, or unexpected triggers, having regular check-ins with a therapist provides accountability and guidance.
For those managing psychiatric medications, medication adherence becomes particularly important in dual diagnosis recovery. Cedar Oaks’ aftercare includes support for maintaining your medication regimen and coordinating with prescribers to adjust treatment as your needs evolve. This ongoing clinical relationship prevents relapse by addressing symptoms before they escalate, giving you the best chance at sustained wellness and freedom from both conditions.
If you or someone you know is struggling with substance use, it’s crucial to seek professional help. Cedar Oaks Wellness offers evidence-based alcohol and drug rehab in Akron, Ohio, helping individuals build a strong foundation for lasting recovery. For more information or to reach out for assistance, please feel free to contact us.
Anxiety affects every part of our lives, causing effects that go beyond just feeling worried or stressed. When anxiety sticks around for a long time, it changes how we think, feel, and go about our daily activities. You might find yourself constantly imagining worst-case scenarios, feeling intense emotions that come and go unpredictably, and avoiding situations that make you uncomfortable.
Common symptoms of anxiety can look different for everyone, but there are some patterns that tend to show up:
These mental health challenges create a cycle where anxiety feeds on itself. You might find yourself avoiding work presentations, declining social invitations, or struggling to make decisions. Sleep becomes elusive, relationships feel strained, and simple tasks can feel insurmountable.
When anxiety takes over, it becomes especially tough to manage your emotions. Your body is always on high alert, making it hard to relax or think clearly. This constant state of being on edge wears out both your mind and body, making it difficult to enjoy the things you used to love and maintain close connections with others.
If you’re dealing with these difficulties and need professional help to get through them, consider reaching out to Cedar Oaks Wellness for support.
Cognitive behavioral therapy is one of the most widely researched and effective approaches for treating anxiety disorders. This evidence-based treatment method operates on the fundamental principle that our thoughts, feelings, and behaviors are interconnected, creating patterns that can either fuel or reduce anxiety symptoms.
The CBT approach focuses on helping individuals understand how their thinking patterns influence their emotions. When someone experiences anxiety, they often develop automatic negative thoughts that can lead to excessive worry or fear. CBT therapists assist clients in identifying these unhelpful thought patterns and evaluating the evidence supporting or contradicting them.
Changing thought patterns is a key aspect of CBT treatment. Instead of accepting anxious thoughts as truths, clients learn to challenge distorted thinking through logical analysis and evidence-based reasoning. For instance, someone who believes “I’m going to fail this presentation and everyone will think I’m incompetent” learns to objectively assess this prediction and cultivate more balanced, realistic thoughts.
CBT sessions usually follow a structured format, lasting 45-60 minutes each. Most anxiety treatment programs consist of 12-20 sessions over several months, although some individuals may experience improvement earlier. Each session includes:
The collaborative nature of CBT empowers clients to become their own therapists, equipped with practical tools they can use long after treatment ends.

Dialectical behavior therapy is a specialized form of traditional cognitive behavioral therapy designed to help people with complex emotional issues. It was developed by Dr. Marsha Linehan in the 1980s, initially for individuals with borderline personality disorder who experienced intense emotions and engaged in self-destructive behaviors.
DBT is based on four main skill areas that work together to bring about lasting change:
Unlike traditional therapy methods that usually involve only weekly sessions, DBT takes a more comprehensive approach. In addition to individual therapy, clients typically participate in:
The emotional regulation skills taught in DBT have been found to be highly effective in treating anxiety, especially when it occurs alongside other mental health conditions. While it was originally created for borderline personality disorder, DBT has also been successfully used to treat various anxiety disorders, depression, eating disorders, and substance use issues.
This holistic approach addresses both the symptoms and underlying emotional patterns that contribute to anxiety, providing a strong foundation for long-term healing.
You might also enjoy: Understanding Manic Depression: Symptoms, Types & Treatment
When exploring CBT vs DBT for anxiety treatment, understanding their distinct approaches becomes crucial for making informed decisions about your mental health journey. These two therapeutic methods, while sharing some foundational elements, diverge significantly in their core philosophies and treatment strategies.
The fundamental difference between these therapies lies in their primary focus and methodology. CBT centers on cognitive restructuring – the systematic identification and modification of negative thought patterns that fuel anxiety. This approach operates on the premise that changing how you think directly impacts how you feel and behave.
CBT’s approach to anxiety involves:
On the other hand, if you’re looking for a more comprehensive approach to mental health that may include addressing deeper emotional or interpersonal issues alongside anxiety, it might be beneficial to consider a program like the Mental Health Treatment in Cincinnati, Ohio – Cedar Oaks Wellness which offers various therapeutic options including CBT and DBT.
DBT takes a different path, emphasizing emotional acceptance alongside change. Rather than immediately challenging anxious thoughts, DBT teaches you to acknowledge and validate your emotional experiences while developing skills to manage them effectively.
DBT’s approach incorporates:
These contrasting philosophies create different treatment goals for anxiety management. CBT aims to reduce anxiety symptoms by eliminating or modifying the thought patterns that trigger them. The goal is symptom reduction through cognitive change, making it particularly effective for specific anxiety disorders like generalized anxiety disorder or panic disorder.
DBT’s goals extend beyond symptom reduction to include emotional regulation and interpersonal effectiveness. For individuals whose anxiety stems from deeper emotional dysregulation or relationship difficulties, DBT provides comprehensive skills training. This approach proves especially valuable when anxiety co-occurs with other conditions involving emotional instability, such as trauma responses or personality disorders.
The choice between these approaches depends on your specific needs, the complexity of your anxiety, and whether additional emotional or interpersonal challenges accompany your symptoms. If you’re considering seeking help, it’s important to find a facility that accepts your insurance provider. For instance, Cedar Oaks Wellness Center is a drug rehab center that accepts Anthem insurance, providing an accessible option for those in need of mental health support.
The structural framework of CBT vs DBT for Anxiety Treatment reveals significant differences in how these therapeutic approaches organize treatment delivery and time commitment.
Cognitive Behavioral Therapy typically operates within a short-term therapy model, with most anxiety treatment programs spanning 12-20 sessions over 3-6 months. This focused timeframe allows individuals to learn cognitive restructuring techniques efficiently, making it an accessible option for those seeking relatively quick relief from anxiety symptoms. Sessions usually occur weekly in individual settings, where you work directly with your therapist to identify and challenge anxious thought patterns.
Dialectical Behavior Therapy follows a long-term therapy approach, often extending 6 months to 2 years depending on individual needs. The structure includes multiple components:
This multi-modal approach emphasizes emotional acceptance alongside skill-building, requiring greater time investment but providing more comprehensive support for complex anxiety presentations.
The intensive nature of DBT’s structure makes it particularly valuable when anxiety co-occurs with emotional dysregulation or interpersonal difficulties, while CBT’s streamlined format serves those with more straightforward anxiety symptoms effectively.
For those seeking such therapeutic interventions in Nashville, local mental health resources such as the ones offered by Cedar Oaks Wellness, a Nashville drug and alcohol rehab center, could be beneficial. They provide holistic programs that may complement traditional therapeutic approaches like CBT and DBT.
CBT shows impressive flexibility in treating various mental health conditions. This therapy method is especially effective for:
DBT takes a different approach, focusing on conditions where emotional dysregulation causes significant life difficulties. Initially created for borderline personality disorder, DBT has broadened its scope to tackle:
The main difference lies in how these therapies deal with comorbid conditions. While CBT excels at targeting specific symptoms through cognitive restructuring, DBT addresses the underlying emotional turmoil that often drives multiple mental health issues simultaneously. This makes DBT especially valuable when anxiety coexists with other complex mental health conditions that require comprehensive emotional regulation skills and emotional acceptance strategies.
The therapeutic objectives for CBT vs DBT for Anxiety Treatment reveal distinct pathways toward healing, each addressing different aspects of the anxiety experience.
CBT centers on symptom reduction through systematic identification and modification of anxious thought patterns. This approach teaches you to:
The goal is direct relief from anxiety symptoms by breaking the cycle of negative thoughts that fuel emotional distress.
DBT takes a broader view, focusing on building comprehensive life skills that address anxiety’s underlying emotional intensity. Through mindfulness practices and emotional acceptance, DBT helps you:
Rather than solely targeting anxious thoughts, DBT recognizes that anxiety often stems from deeper emotional dysregulation patterns. The therapy teaches you to surf emotional waves skillfully, creating space between intense feelings and reactive behaviors that might worsen anxiety in the long term.
Moreover, it’s worth noting that both CBT and DBT have been shown to effectively treat various forms of anxiety, offering valuable insights and tools for those struggling with these conditions.
CBT typically serves as the preferred initial approach for individuals experiencing straightforward anxiety disorders. This therapy works exceptionally well for people who can identify specific triggers and thought patterns contributing to their anxiety. Those experiencing generalized anxiety, social anxiety, or panic disorder often respond positively to cognitive restructuring techniques that challenge irrational fears and catastrophic thinking.
DBT proves more suitable for individuals facing complex emotional challenges beyond basic anxiety symptoms. People struggling with emotional dysregulation, intense mood swings, or self-destructive behaviors benefit from DBT’s comprehensive skill-building approach. This therapy becomes particularly valuable for those requiring dual diagnosis treatment, where anxiety coexists with conditions like borderline personality disorder, substance use disorders, or trauma-related issues.
The mindfulness and emotional acceptance components of DBT provide crucial support for individuals who feel overwhelmed by the intensity of their emotions, making traditional cognitive approaches feel inadequate or invalidating.
Every person’s anxiety manifests differently, requiring personalized treatment plans that honor their unique circumstances. A thorough clinical assessment examines not only anxiety symptoms but also emotional regulation patterns, relationship dynamics, and coping mechanisms. This comprehensive evaluation helps determine whether CBT’s focus on thought modification or DBT’s broader emotional skills training will create the most meaningful path toward healing and recovery.
For those seeking more intensive support, understanding how to find an inpatient mental health treatment center can be a crucial step in their recovery journey.
Many skilled therapists recognize that healing doesn’t always follow a single path. Combined therapy approaches often begin with CBT techniques to address immediate cognitive patterns contributing to anxiety. When clients struggle with intense emotional responses or have difficulty implementing traditional CBT strategies, therapists may gradually introduce DBT skills to strengthen emotional regulation capabilities.
This flexible therapeutic approach offers several meaningful advantages:
Holistic mental health care recognizes that anxiety rarely exists in isolation. At comprehensive treatment centers, therapists assess each person’s unique presentation and may seamlessly blend techniques from both modalities. Someone experiencing panic attacks might benefit from CBT’s exposure techniques while simultaneously learning DBT’s grounding exercises for emotional regulation.
For individuals grappling with anxiety alongside substance use disorders, West Virginia Addiction Treatment Guide can provide valuable resources. The therapeutic relationship becomes a collaborative space where you and your therapist can explore which combination of strategies feels most supportive. This personalized approach acknowledges that your healing journey is unique, and the most effective treatment plan may draw from multiple evidence-based approaches to address both the cognitive and emotional aspects of anxiety.
Mental illness affects millions of people worldwide, manifesting through various symptoms that impact daily life. These conditions can alter your thoughts, emotional responses, and behavioral patterns in significant ways:
Depression stands as one of the most prevalent mental health challenges, carrying an invisible weight that affects every aspect of life. You might experience:
Psychiatric emergencies can escalate quickly, disrupting your ability to function. Warning signs include:
For those experiencing panic disorder, these symptoms can be particularly severe and require immediate attention. Treatment options are available at specialized centers like Cedar Oaks Wellness.
The challenge becomes more complex with dual diagnosis – when mental health issues occur alongside substance use disorders. This combination requires specialized treatment approaches such as integrated therapy addressing both conditions, medication management, support group participation, lifestyle modifications, and regular monitoring of treatment plans.
Moreover, specific mental health conditions like personality disorders also necessitate tailored treatment strategies which are offered at facilities like Cedar Oaks Wellness.
If you or a loved one is struggling with these issues and are considering seeking help, understanding the admissions process at Cedar Oaks Wellness Center can be a helpful first step towards recovery.
Mental health therapists are licensed professionals with specialized training in psychological treatment and counseling. Here’s what you need to know about different types of therapists:
These professionals provide various therapeutic services:
Each type of therapist brings unique skills and approaches to mental health treatment, allowing you to find the right match for your specific needs. In some cases, inpatient mental health treatment may be necessary. If you’re seeking such a facility, it’s essential to know how to find an inpatient mental health treatment center that best suits your needs.
For those considering such options, Cedar Oaks Wellness offers valuable resources and assistance in navigating these challenging circumstances.
Finding qualified mental health professionals in your area has become easier with digital resources. Popular platforms like Psychology Today, GoodTherapy, and TherapyTribe maintain extensive directories of licensed therapists.
These platforms offer specific search filters to match your needs:
Many therapist directories include detailed profiles with professional photos, treatment philosophies, and client reviews. You can often schedule consultations directly through these platforms to assess your comfort level with potential therapists.
Local medical centers and community health organizations also maintain lists of mental health providers in your area. These resources can help connect you with therapists who understand your community’s specific needs.
Getting mental health support shouldn’t break the bank. Many therapists accept major insurance plans, including Medicare and Medicaid. You can verify insurance coverage by:
No Insurance? Here Are Affordable Options:
Some therapists offer payment plans or discounted packages for multiple sessions. Local non-profit organizations and religious institutions might provide free or low-cost counseling services. Universities with psychology departments often run research studies offering free therapy in exchange for participation.
The National Alliance on Mental Illness (NAMI) maintains lists of affordable mental health resources in most communities. Your local health department can direct you to subsidized mental health services.
In addition to traditional therapy, there are also specialized options available for those struggling with substance abuse. For instance, drug treatment programs often provide a range of services that are both accessible and affordable.
Local therapists offer diverse treatment approaches tailored to your specific needs. Individual therapy provides one-on-one sessions where you can work through personal challenges with undivided attention from your therapist. Group therapy creates a supportive environment where you can connect with others facing similar struggles while developing coping skills.
Many local therapists offer specialized services to address specific mental health concerns. Here are some of the common therapies you may find:
In addition to individual therapies, many local providers also offer specialized programs for certain conditions or populations. These programs may include:
Therapy services can be delivered in various ways to accommodate different preferences and needs. Here are some common delivery methods:
It’s important to discuss your preferences with potential therapists to ensure they can provide the type of service that suits you best.
Selecting the right mental health therapist requires careful evaluation of several key factors. Your therapist’s credentials serve as the foundation of their expertise – look for state licensure, professional certifications, and advanced degrees in psychology, counseling, or related fields.
Consider therapists who specialize in your specific concerns:
Practical considerations play a vital role in successful therapy:
Match your therapist’s treatment approach with your preferences. Some practitioners focus on solution-based strategies, while others explore deep-rooted patterns. Ask potential therapists about their methodology and ensure it aligns with your goals and comfort level.
Stress management is a crucial part of mental health therapy. Mental health therapists teach you practical techniques to cope with daily pressures:
Your therapist helps identify stress triggers in different areas of your life:
These personalized strategies build resilience and create sustainable lifestyle changes. Your therapist tailors these techniques to suit your specific needs, ensuring you develop a practical stress management toolkit that fits into your daily routine.
Regular therapy sessions provide a safe space to practice these coping mechanisms and refine them based on your progress. This structured approach helps you maintain mental wellness while dealing with life’s challenges.
For those struggling with more severe mental health issues, such as bipolar disorder or addiction, it’s important to seek specialized help. In such cases, exploring local resources like those offered by Cedar Oaks Wellness in Nashville or Toledo could provide the necessary support. They offer holistic programs that not only address addiction but also incorporate essential stress management techniques into the recovery process.
Hospital-based mental health services offer integrated treatment options that combine various therapeutic approaches under one roof. Your local healthcare systems typically provide:
Behavioral health providers work as part of coordinated care teams to deliver personalized treatment plans. This collaborative approach includes:
Many local hospitals maintain networks of mental health professionals who specialize in specific conditions. These specialists can address complex cases requiring multiple treatment modalities – from cognitive behavioral therapy to medication-assisted treatment for dual diagnosis.
For instance, if you’re dealing with a hoarding disorder, there are specialized centers in Ohio that focus on such conditions. Your treatment team will work together to monitor progress, adjust approaches, and ensure you receive comprehensive support throughout your mental health journey.
Additionally, if you or someone you know is struggling with addiction, resources like the Indiana Addiction Treatment Guide can be invaluable. They navigate the complex world of addiction and mental health treatment, providing adequate resources.
For those specifically in the Indianapolis area seeking help, there are addiction treatment options near Indianapolis that offer personalized care and support for lasting recovery.